Building an Objective, Lower-Cost and Portable Glaucoma Screening Tool
By Tiffany Fox
Note: This is the third in a three-part series about Qualcomm Institute research projects that have a direct impact on aging. (Read the first two stories here and here). All three projects are funded through the Calit2 Strategic Research Opportunities program. The Qualcomm Institute is the University of California, San Diego division of the California Institute for Telecommunications and Information Technology (Calit2).
San Diego, Calif., Oct. 23, 2014 — Glaucoma is the leading cause of irreversible blindness in the world, affecting more than 80 million people. However, because the disease remains largely asymptomatic as it progresses, researchers estimate that more than 50 percent of individuals are unaware that they’re afflicted until it’s too late.
To make matters worse, there are is no effective way to screen for the disease. The current diagnostic process -- which requires patients to have the forethought to make an appointment -- is subjective, cumbersome and expensive, says Felipe Medeiros, professor of Ophthalmology and the Ben and Wanda Hildyard Chair for Diseases of the Eye at the University of California, San Diego.
Medeiros is hoping the new diagnostic tool he’s developing in collaboration with the Qualcomm Institute will provide an objective, low-cost and even portable means for screening patients for visual field loss and glaucoma.
“The way we currently assess visual function in these patients is with Standard Automated Perimetry (SAP), which evaluates loss of vision by requiring the patient to press a button to indicate whether or not he or she has seen a series of very dim visual stimuli,” he explains. “This test has a number of limitations – not only must patients come into a physician’s office to be tested, but the testing process is fatiguing, difficult and tedious. It’s also subject to a lot of variability and learning effects.”
“It’s not an easy test for patients to do,” he continues, “but it’s pretty much all we have, not only for glaucoma but for other diseases that can affect the visual field.”
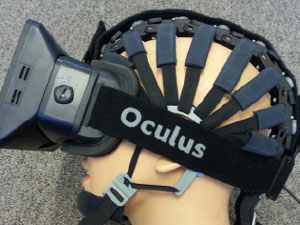
Medeiros’ proposed replacement combines head-mounted virtual reality goggles typically used for video games with a wireless dry Electroencephalogram (EEG) system to measure the electrical field changes associated with processing visual field stimuli. The testing platform is based on objective analysis of the EEG signals and therefore does not require subjective responses from the patient. The data can be transmitted to a smartphone or tablet device, making for easy retrieval and analysis by clinicians.
Medeiros received a $50,000 Calit2 Strategic Research Opportunities (CSRO) grant earlier this year to build a proof-of-concept of the device, which he and his team will use to conduct preliminary investigations of its worth as a diagnostic tool.

Notes Medeiros: “Because the equipment is portable and doesn’t require much set-up, testing could be done much more easily, maybe even at a patient’s home or in certain underserved locations where there are no machines that can conduct the SAP test.
“Furthermore, having a more objective test may decrease variability and increase reproducibility. In addition to its use in screening for visual field loss, the test could also potentially be used to monitor glaucoma patients over time. Think about having a device that you could use to test yourself many times throughout the year, providing data from 10 or more tests per year. We cannot do this for SAP.”
Medeiros is partnering with neuroscientist and Swartz Center of Computational Neuroscience Co-Director Tzyy-Ping Jung to develop the system and incorporate algorithms that will parse the brain signals associated with visual stimuli from among all the diverse signals captured by the EEG.
The team has already begun collecting preliminary data on control subjects (those without signs of glaucoma) as well as a large cohort of patients with glaucoma who are part of a longitudinal study at the UC San Diego Shiley Eye Center.
Media Contacts
Tiffany Fox, (858) 246-0353, tfox@ucsd.edu
Related Links